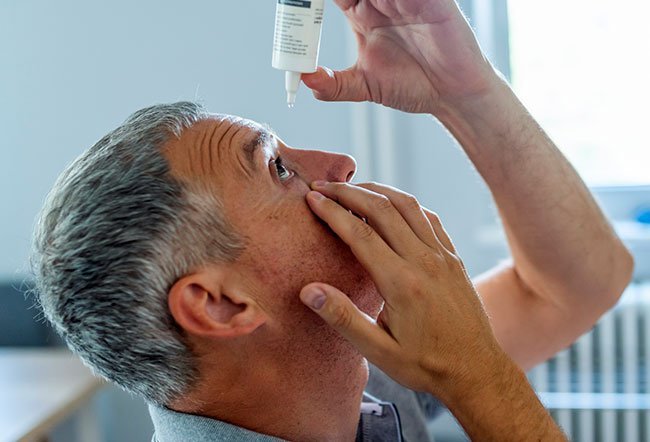
Sjogren’s syndrome or sicca syndrome is an autoimmune disease in which dry mouth and eyes are usually the first manifestations of a complex chronic process. We explain what causes it.
Sjogren ‘s syndrome is also known as ‘ syndrome dry ‘. It is an autoimmune disease in which xerophthalmia –ocular dryness– and xerostomia –dry mouth– appear as fundamental symptoms. Additionally, the patient with Sjögren’s syndrome may have many other manifestations of multiple organs.
This pathology affects around 120,000 people in Spain, according to the Spanish Association of Sjögren’s Syndrome, and can be primary or be associated with other autoimmune diseases.
Sjogren’s syndrome does not have a single cause, although it does appear in individuals with a genetic predisposition. Even so, no analysis allows predicting which people will suffer it. The initial symptoms are usually dry mouth and eyes that can last for years without consulting a doctor.
Over time, being a chronic disease, many complications can appear in different organs and a significant decrease in the quality of life of the affected person.
It is much more common in women. Thus, for every male affected by Sjögren, there are nine sick women. The first symptoms usually appear between the ages of 40 and 60, although sometimes the diagnosis can be delayed for years.
The exact incidence is unknown because it varies significantly by age, sex, and race and because the diagnostic criteria have changed over the years. Still, it is considered that between 0.5% and 4% of adults suffer from it.
Unfortunately, there is no effective treatment to cure the disease, which has a chronic course. Nor can you stop its system or slow it down. However, there are measures to control the symptoms, although they are often insufficient to achieve a complete improvement of the problems suffered by the patient.
This means that the quality of life of those affected can be significantly affected, not only because of how annoying the continuous sensation of dry mouth and eyes is but also because it can be accompanied by severe complications that darken the prognosis in cases that appear.
Proper monitoring by a doctor who is an expert in Sjogren’s syndrome – usually a rheumatologist who is an expert in autoimmune disease – will allow the possible complications to be detected and treated appropriately and early. The collaboration of the ophthalmologist is also essential to address eye problems that patients may present. There are also patient associations that support those affected and their families.
Causes of Sjögren’s syndrome
There are two forms of Sjogren’s syndrome: primary and secondary. The primary one is a chronic progressive inflammatory autoimmune endocrinopathy. This means that the exocrine glands (those that make tears, saliva, sweat) are affected by an inflammatory autoimmune process. The disease is triggered because the body itself manufactures substances that attack cells of these glands and produce inflammation of the same (with a lymphocyte-type infiltrate).
The primary Sjogren syndrome has autoimmune diseases in general, a multifactorial base. Among these causes, in the first place, there must be a genetic predisposition or susceptibility to suffering from the disease.
Primary Sjögren’s syndrome is a polygenic-based disease. That is, a single gene does not produce it. In Caucasians, it is associated with the HLA-DR3 genes. The TAP1 and TAP2 genes also increase the predisposition to suffer from this pathology. Despite this genetic predisposition, Sjögren’s syndrome is not considered a hereditary disease, although it is more common in relatives of people with autoimmune connective tissue diseases.
There are then alterations in the mechanisms that regulate apoptosis (it is programmed cell death) on this genetic predisposition. It could be that some virus or external toxin participated in this process. In addition, another cause of Sjögren ‘s syndrome is that an imbalance of various inflammatory substances occurs together with the infiltration of lymphocytes (first type T and then type B) in the affected glands.
The epithelium itself also participates in inflammation. In short, it is a complex phenomenon in which genes, possible external factors, the cells of our immune system, and various substances that promote inflammation interact.
As for secondary Sjögren’s syndrome, it is the one associated with other systemic autoimmune diseases. Systemic lupus erythematosus, rheumatoid arthritis, and scleroderma are autoimmune diseases that occur most frequently.
On the other hand, Sjögren-like syndrome appears in some patients with HIV infection or the hepatitis C virus.
Furthermore, celiac disease (like other autoimmune diseases) may also be associated with Sjögren’s syndrome in a higher proportion than in the general population.